Diabetic Foot Care
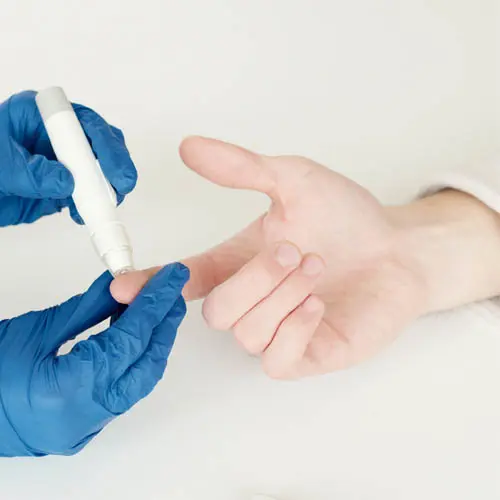
Diabetes is one of the most common chronic adult illnesses. When your blood sugar is out of control, you have a higher risk of foot complications. For example, you can develop diabetic foot. This condition is caused by poor circulation and nerve damage, leading to wounds, infections, and amputations in the most severe cases.
Controlling your blood sugar is essential to avoid complications involving your feet and legs. Next is finding the right podiatrist specializing in diabetic foot care, like Dr. Cameron. Together with his team at Foot and Ankle Center, he can perform routine exams with your baseline benchmark to measure improvement and degradation better than you may be able to at home. He can provide early interventions, education, and care to prevent problems from developing into more severe conditions. Take proper care to avoid these diabetic complications:
Diabetic Neuropathy
High blood sugar can cause this nerve disorder anywhere in your body. You often experience numbness, tingling, and burning sensations in your feet and lower legs.
You can also have muscle weakness, which leads to more injuries. If you haven’t had neuropathy symptoms, control your blood sugar to avoid it. This will also prevent progression and further nerve damage if you already have some pins and needles.
Gabapentin and pregabalin are the go-to medications for diabetic neuropathy treatment. Topical creams and gels can also reduce pain and improve nerve function temporarily.
Physical therapy can help you reduce your risk of falls by focusing on balance, coordination, and strength-training exercises. Diabetic podiatrists recommend transcutaneous electrical nerve stimulation (TENS) therapy as it effectively improves nerve function and reduces pain from the comfort of your home.

Charcot Neuroarthropathy
Due to the loss of sensation from neuropathy and decreased blood flow, you can also develop a condition called Charcot foot for pronunciation ease.
It’s a destructive degenerative disease for your bones and joints, leading to sometimes irreparable structural foot changes. Early symptoms can be subtle and difficult to detect. If you have diabetes and suffer a stress fracture, Charcot foot could be the cause.
You can encounter deformity, instability, and chronic pain if left too long. If you detect any redness, swelling, or tenderness, especially with foot shape changes or difficulty walking, seek medical attention immediately.
Diabetic Ulcers
Medical professionals may refer to them as neurotrophic ulcers. They typically occur on the soles of your feet. Up to 25% of patients with diabetes will develop ulcers, according to the National Institute of Health.
If your blood sugar is too high, it damages your blood vessels and leads to circulation problems. Coupled with nerve damage or neuropathy, you won’t be able to feel when your shoes are too tight or rubbing, leading to frequent blisters and cuts.
While benign for someone without circulation problems, your body won’t be able to heal as efficiently. Since you need to continue to use your feet in shoes daily, diabetic ulcers become almost inevitable.
Daily inspection is crucial to help prevent skin breakdown from turning into these open sores.
Even if you cannot see changes, feel your feet closely for swelling, burning, and pain, as they are indicators of an ulcer brewing. Without swift intervention, ulcers will quickly turn into infections.


Diabetic Infections
Diabetes puts you at higher risk for infections. You can have bacterial or fungal infections that can develop into abscesses, pus-filled pockets that require draining and antibiotics. They can also turn into several invasive conditions:
- Cellulitis is an infection that’s spread to the surrounding skin and fat layers, needing heavy antibiotics.
- Osteomyelitis is similar to cellulitis, but it’s spread to the bone. Incredibly dangerous, you want to treat infections before they infect your bones.
- Gangrene: while not an actual infection, this can occur due to them. Tissue death occurs when its blood supply is interrupted by infection or other trauma, compounded by already poor circulation from diabetes. Doctors cannot save the tissue; a surgeon must remove it to help you heal.
When infections become too great, or gangrene has started, your doctors may recommend amputation. It’s crucial to follow diabetic foot care prescribed by your doctor or podiatrist to avoid these awful outcomes.
Diabetic Foot Care
1. Invest In Good-Fitting Socks and Shoes
Your socks should be breathable from a natural fiber like cotton or bamboo to wick away sweat. Your shoes should fit comfortably in length and width to avoid rubs or trouble spots. Stiff dress shoes, pointed or open toes, flip flops, and high heels are all more prone to harm your feet. Look for enough ankle and arch support to stand comfortably for a few hours.
2. Clean and Dry Your Feet Daily
Wash your feet with warm water and soap. Ensure they are completely dry before putting on socks and shoes, especially between your toes. Moisturizing your feet isn’t bad, as it prevents dry skin from leading to more cuts. However, avoid it between your toes, as the increased moisture can lead to fungal infections.
3. Perform Routine Inspections
While washing your feet, it’s a good time to do a daily once-over. You want to check for swelling, tenderness, or skin changes. You should watch out for redness or painful spots. If you find any cuts, blisters, or sores, you want to clean and dress them to prevent ulceration.
In addition to inspecting your feet, you should check your shoes before use. Look for any breakdown or sharp areas that can cause injury. Keep an eye out for pebbles or other debris in your shoes that can hurt your feet while wearing them.
4. Protect Your Feet
Avoid going barefoot at all costs. Even inside, wear fluffy socks with grips or house slippers at a minimum. Wear hiking boots or other protective footwear in wet, uneven, or unknown terrain to prevent stubbed toes, prolonged wet feet, or other injuries that can lead to complications.
The reduced sensation can make it hard for you to detect when your feet are too cold or hot. Check the weather and wear appropriate socks for the temperature and length of your excursion. For example, thinner cotton socks for summer outings and thick wool socks for winter days. Avoid foot warmers, as you won’t be able to tell when they are burning your toes.
5. Rest and Elevate
Build in rest for your feet and legs, especially if you’re standing or walking for long periods. Even if there isn’t any apparent swelling, elevate your feet to promote circulation and reduce inflammation. Wearing prescription stockings or socks can help reduce fatigue and inflammation and aid circulation.
6. Learn How To Cut Your Nails
Trim your toenails carefully. They should be cut straight across and filed to prevent rough edges. If you cut them too short, you can cause ingrown toenails and infections. Often, a diabetic podiatrist will trim your nails for you to avoid unnecessary risk.
7. Control Your Blood Sugar
Whether you control your blood glucose levels through diet, medications, or a combination, commit yourself to the treatment plan. Uncontrolled blood sugar is a quick way to get ulcers, neuropathy, or worse.
8. Reduce Substance Use
Drinking alcohol wreaks havoc on your blood sugar if you have diabetes. It initially drops your blood sugar but then stimulates your liver to produce and release more glucose. When you are trying to keep your blood sugar within a stable range with diet or short-acting insulin, alcohol makes it challenging.
Unfortunately, alcohol can interact with your diabetes medications, making them less effective over time. It also dehydrates you, putting more strain on your cardiovascular system and internal organs. Try to minimize your alcoholic beverages as much as possible.
Smoking is another habit that can negatively affect blood sugar control and diabetes. Long-term smoking leads to insulin resistance, increasing your risk of type 2 diabetes if you don’t already have it. Because it contributes to higher blood sugar levels, it worsens your blood sugar control and diabetes symptoms.
Nicotine also makes the walls of your blood vessels sticky, limiting blood flow through congestion. This harms your healing power and increases your risk of developing complications like nerve damage, diabetic foot, cardiovascular disease, and stroke.
Why Foot and Ankle Center Should Provide Your Diabetic Foot Care
With real and dire threats of ulcers, infections, and amputation, having an experienced diabetic podiatrist on your treatment team is crucial. Dr. Cameron has provided treatments for foot ailments such as diabetic neuropathy for over ten years. As a top foot and ankle specialist in the region, he can help you in many ways:
Examine Your Feet Regularly and Provide Care
Dr. Cameron has the training, knowledge, and experience to examine your feet and detect any signs of damage or concerning areas.
He can check your circulation, sensation, and range of motion to be proactive in your treatments for diabetic neuropathy, decreased circulation, and anything else that could lead to further problems.
Provide Education on Home Care
Dr. Cameron truly enjoys spending time with his patients, getting to know them all to help them more effectively.
Without getting to know you, he would never learn that you prefer to wear high-heeled shoes for your ballroom dance hobby, for example, which contributes to all your feet problems.
With this extra time, he makes a point to provide supplementary education on managing your diabetes and caring for your feet properly at home. He covers your footwear, proper foot hygiene, and self-examination techniques, so you don’t have to depend on his expertise during office visits.
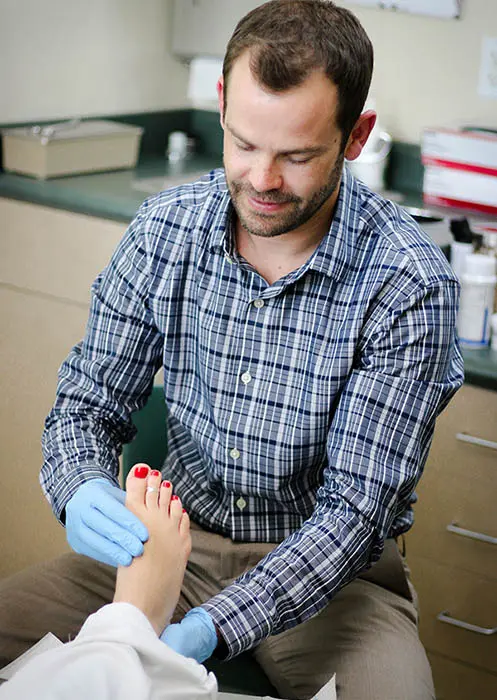
Prevent Diabetic Foot Complications
By taking the time to conduct thorough exams and histories extending beyond your medical record and giving you extensive diabetic foot care education, Dr. Cameron goes above and beyond to prevent complications. He will also encourage proper glucose management and a healthy lifestyle to avoid further issues.
Treat Foot Problems
If Dr. Cameron detects any potential issues, he can provide swift treatment to prevent them from progressing. He can prescribe custom orthotics, shoes, and medications depending on the problem. He can provide wound care and home instructions to avoid frequent clinic visits for dressing changes and drain abscesses if required.
Since he is a board-certified foot and ankle surgeon, he can personally take care of any of your surgical needs, minor or significant, involving your lower leg. However, his goal is to help with your diabetes management so you never need surgical intervention.
Overall, having a diabetic podiatrist as a healthcare team member is vital, providing education, tips, and specialized interventions to improve your quality of life. Living with a chronic condition is difficult enough without having to suffer the pain of debilitating neuropathy or frequent ulcers. Schedule a consult with Dr. Cameron today.
